This advertorial is sponsored by Tampa General Hospital.
The Aortic Disease Program at Tampa General Hospital’s Heart & Vascular Institute is no stranger to the challenges of complex care. Situated in the population center of Tampa, Florida, in the nation’s third most populous state, the tertiary referral center stands poised to meet the flow of incoming cases that show increasing degrees of complexity.
The times could not be more apt for the team’s collaborative approach. Tampa General Hospital performs a large volume of fenestrated endovascular aneurysm repairs (FEVARs) for abdominal aortic aneurysms (AAAs) compared to many other centers, and confronts a familiar problem, says Dean Arnaoutakis, MD, the medical director of the Tampa General Hospital Aortic Disease Program. The combination of a large elderly population with increased implementation of EVAR over the past decade has given rise to the increasingly common patient, popping up across the country, who presents with aneurysm sac growth, despite prior EVAR.
“We’ve done over 100 FEVARs in the last year,” observes Arnaoutakis, also an associate professor of surgery at the University of South Florida. “And about a third of that volume is for patients who have had failed prior EVARs, typically from a type I endoleak. So, we are amounting a rather robust experience and program of salvaging old EVARs by putting in custom fenestrated endograft to obtain more appropriate proximal aortic seal.”
This facility for endovascular salvage for prior failed EVARs is the result of a well of experience navigating the specific anatomic nuances and pathology of these complex cases. Though these EVAR revisions are showing up all across the U.S, Arnaoutakis sees a higher overall number owing to being at one of the region’s largest tertiary referral centers in addition to the large elderly population in the area, many of whom are former or active smokers, and thus more likely to have had an EVAR implanted in the first place.
Besides revisions linked to EVARs originally performed outside of instructions for use parameters, Arnaoutakis also points to the volume of cases he carries out related to older iterations of aortic stent grafts. “Previously published studies indicate that compliance with EVAR implantation guidelines is poor with up to 40-60% implanted off-label,” he says, which “will naturally lead to that device failing over time. I think we are now seeing more of these cases now.
“In addition, we’re seeing a lot of first-generation devices, which are more than 10 to 15 years old, fail. We have learned over time that these earlier generation devices have either design or material imperfections. These issues are driving the high rate of failed EVARs in our practice.”
Arnaoutakis himself has been working to help find ways of dealing with these types of cases. One is a physician-sponsored investigational device exemption (PS-IDE) he gained earlier this year from the Food and Drug Administration (FDA) to evaluate the efficacy of fenestrated and branched EVARs using physician-modified endografts (PMEGs) in a clinical trial setting. “There were many reasons to apply for a PS-IDE to do F/BEVAR with PMEGs. The number of patients I encountered with failed prior EVAR who would not tolerate an open explant was certainly a driving factor as the current FDA-approved fenestrated device is typically not usable in this setting due to constraints with the device design. These patients often require a four-vessel fenestrated device with complete relining of the prior endograft, a device which is currently not commercially available,” he explains.
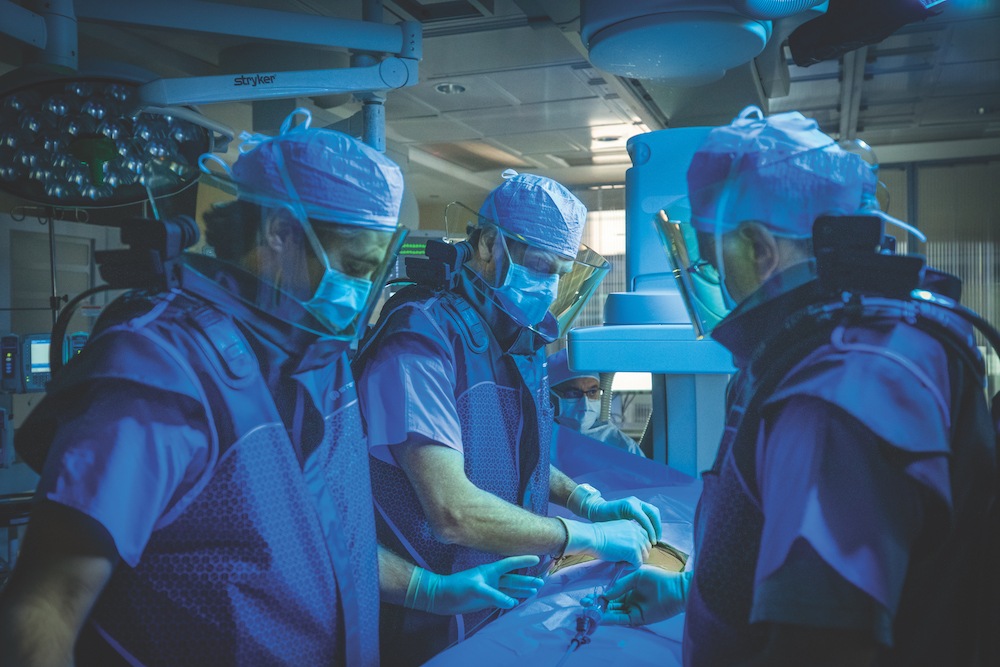
Increasing complexity, of course, comes with the inherent dangers posed by exposure to higher doses of radiation. In order to mitigate the effects, team members carrying out these procedures have access to zero-gravity, lead-based suits designed to decrease the amount of radiation to which they are exposed—which is “considerable” in the context of 100-plus FEVARs per year, Arnaoutakis points out. Similarly, the team uses cloud-based fusion imaging technology, which also helps reduce radiation exposure and speeds up procedural times, to make them more efficient and safe, he adds.
Arnaoutakis and the multidisciplinary Tampa General Hospital aortic team are well poised to deal with the incoming volume of these complex cases. “As our fenestrated endovascular aortic program has become more sophisticated, our overall practice has evolved such that we can salvage these failed endografts, which is decreasing our number of open explant operations. Our preliminary data suggests that this evolution in our practice has improved our patient outcomes,” he says.
That multidisciplinary team—previously led by Murray Shames, MD, now Tampa General Hospital’s chief of staff and the Richard G. Connar Endowed Professor and chair of surgery at the University of South Florida—includes key members from vascular surgery and interventional radiology. “We have a wonderful relationship with our interventional radiologists here who we often do these operations in conjunction with,” notes Arnaoutakis. “We each have a slightly different skillset, and, when combined, it really promotes our procedure technical success and improves patient outcomes.”












