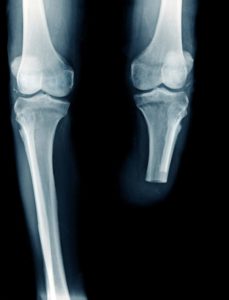
A recent study, published online in the European Journal of Vascular and Endovascular Surgery (EJVES), found that regional anesthesia alone is reasonable for major lower extremity amputation (LEAMP) in high-risk patients, and may initiate a more efficacious enhanced recovery program than general anesthesia.
The authors of this retrospective cohort study—Michael R. Hall, MD, of the University of North Carolina at Chapel Hill, et al—detail that there was no difference in outcomes between regional or general anesthesia techniques in patients undergoing LEAMP, but add that further studies are needed to establish best practices in LEAMP procedures.
Hall et al emphasize the fact that major limb amputations are psychologically stressful and subject patients to perioperative cardiovascular risk. They note that up to 90% of major LEAMP are being performed under general anesthesia, despite the fact that regional anesthesia is an acceptable option in most cases.
The authors state that obtaining a better understanding of who would benefit from regional versus general anesthesia could reduce complications and help to establish best evidence-based practice, and their hypothesis was that patients undergoing LEAMP with regional anesthesia would have better postoperative outcomes than patients receiving general anesthesia.
Hall and colleagues used the Vascular Quality Initiative (VQI) lower extremity amputation module to identify patients aged 18 or over who underwent LEAMP from 2013 to 2018.
They note that outcomes included 30-day incidence of major adverse cardiac events (MACE) and all-cause mortality, and used multivariate logistic regression modules to compute odds ratios (ORs) and 95% confidence intervals (CI). They analyzed time to death using standard survival analysis.
Writing in EJVES, Hall et al detail that the final sample included 5,567 patients (median age: 65 years; 67% white, 65% male). They report that only 719 patients, representing 13% of the cohort, received regional anesthesia. In addition, compared with patients undergoing general anesthesia, patients in the regional group were older (67 vs. 65 years; p<0.001) and more likely to have diabetes (78% vs. 69%; p<0.001), end stage renal disease (26% vs. 18%; p<0.001), congestive heart failure (33% vs. 27%; p<0.01), and coronary artery disease (35% vs. 30%; p<0.01).
Hall and colleagues add that the overall incidence of MACE, death, and MACE or death was 5%, 6%, and 9%, respectively. In addition, there was no statistically significant difference by anesthesia groups for MACE (OR 0.98, 95% CI 0.69–1.39) or mortality (hazard ratio [HR] 1.03, 95% CI 0.9–1.17).
According to Hall et al, this is the largest retrospective study analyzing the outcomes for LEAMP using either regional or general anesthesia. They note that other research using the National Surgical Quality Improvement Program (NSQIP) database demonstrated similar results, namely no difference in 30-day mortality or cardiac events, but was limited to above-knee amputations only and the majority of the regional anesthesia used was spinal anesthesia. “The present results parallel these studies while including regional nerve block techniques as well as all major LEAMP in the analysis,” they comment, which they add suggests acceptable short-term outcomes for all types of regional anesthesia.
The authors recognize that physiological stress during and immediately after the major LEAMP operation may drive the postoperative outcomes regardless of anesthetic approach and state that further study is warranted to determine whether regional anesthesia can attenuate that stress by reducing the pain response during and after surgery.
Hall et al also acknowledge that the study is observational in nature and so the results do not imply causality, but instead describe the association between anesthesia type and outcomes.
Commenting further on the study design, they concede that it made controlling for residual confounding impossible. “A randomized trial would be required to address this issue,” they remark.
Hall and colleagues end by stressing the many strengths of the methods they used. “The VQI represents a ‘real-world’ data source that provides a view of current outcomes in a large population of patients undergoing elective limb amputation,” they comment, and the findings “offer a critical insight into this highly complex, highly comorbid, and understudied population.”
The authors conclude that many patients are candidates for regional anesthesia and this study “has shown that his method of anesthesia is a reasonable alternative to general anesthesia.”












