In the ascending aorta session at CX Aortic Vienna, presentations focused on various treatment options, including frozen elephant trunk (FET) and endovascular intervention. The panelists emphasized the scarcity of data in this zone and called for data gathering. Simultaneously, the discussion highlighted the near impossibility of conducting randomized controlled trials due to small patient numbers and the fact that few operators have substantial experience in this area, among other factors.
This session, and all other sessions from day one of CX Aortic Vienna, is available to view on demand. Click here to register and access the recording.
Opening the session, Rodney White, MD, of Long Beach, California, gave a presentation on the evolving indications of ascending aortic endografts and their limitations. He detailed that preliminary evaluation of modified Valiant thoracic endografts (Medtronic) for ‘tubular’ ascending aortic lesions, including ascending dissections. He added that tortuous ascending aorta can lead to underestimation of length required for complete coverage of outer wall, and that a transapical approach is being considered as a better alternative for ‘horizontal heart’ configurations.
Speaking on aortic root replacement surgery in patients with coronary artery disease (CAD), Joseph Coselli, MD, of Houston, argued that strategies specifically targeted to patients with CAD are needed. “Patients with CAD undergoing aortic root replacement are older, have diminished health, face complex repair, and have worse outcomes than those without,” he detailed, adding that while CAD per se is not a predictor of death, Kaplan-Meier analyses suggest that patients with CAD have poorer survival than those without.
Michael Jacobs, MD, of Maastricht, The Netherlands, touched on the subject of staged procedures for multilevel aneurysms in the aortic arch and thoracoabdominal aorta. Summarizing, he told registrants that in the open and endovascular repair of complex, very extensive aortic aneurysms, his advice would be to stage. If technically feasible, he advised to start with the most “threatening” part first, which will be in either the chest or in the abdomen, and recommended an interval between the two procedures of around four weeks. He detailed that a gap of four weeks is needed to develop spinal cord collateral vasculature. Jacobs ended by warning that there is a potential danger of aneurysm rupture in between stages.

Turning the attention of the audience to dissection, Luca Bertoglio, MD, of Milan, Italy, spoke on the open and endovascular treatment options for aortic downstream pathology after FET. He concluded that FET is an optimal solution when any kind of distal thoracic procedures are planned and stressed that a multidisciplinary approach is key to improve results and plan patient-tailored solutions.
Donald Adam, MD, of Birmingham, U.K., discussed distal open and endovascular aortic reconstruction after total arch repair with FET. He noted that there is limited outcome data on the subject and that surveillance is mandatory to avoid distal rupture. In addition, he relayed that open and endovascular repair are complementary approaches. “Any centre performing frozen elephant trunk must be able to provide both options,” he remarked, adding that multicenter studies are required to define indications and outcomes.
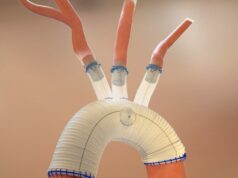
Finally, Eric Roselli, MD, of Cleveland, informed registrants how and when to use branched stented anastomosis FET repair, or the B-SAFER procedure. “In general, this is a very versatile approach to complex arch disease,” he remarked. Roselli summarized that the most efficient form of the B-SAFER is the single anastomosis, single stent iteration. For patients with arch aneurysm, however, he noted that the Cleveland Clinic team will often add multiple anastomoses, or if the branches are anomalous or diseased, they may add multiple stents or use a combination of both of these pools to create a faster and hopefully safer arch reconstruction.