Vascular surgeons in private practice could play a crucial role in alleviating one of the existential problems currently vexing the specialty: The training of future generations of specialists and its intersection with declining numbers of open abdominal aortic aneurysm (AAA) repairs.
The ability of those in private practice to contribute to the total number of training positions available across the United States, as well as to broaden the church of open aortic cases available for trainee involvement amid the fall in AAA repairs performed surgically, was brought into sharp focus during a training and education scientific session held during the 2022 Annual Symposium of the Society for Clinical Vascular Surgery (SCVS) in Las Vegas (March 19–23). Discussion was stirred by data delivered by Malachi Sheahan III, MD, on the success of a national initiative carried out to explore how to overcome barriers and better help those interested in starting new vascular training programs, as well as new statistics presented by Thomas F. X. O’Donnell, MD, that showed the “significant proportion” of open AAAs completed without any trainee participation.
Sheahan, chief of vascular surgery at Louisiana State University (LSU) in New Orleans, told SCVS attendees how since he was charged with helping spark an increase in vascular training programs in 2019, his research had demonstrated a sharp increase to 28 new programs in the last three years—compared to just seven in the three years prior.
Working under the auspices of the Society for Vascular Surgery (SVS) and the Association of Program Directors in Vascular Surgery (APDVS), he and colleagues on a taskforce formed for the initiative reached out to 172 general surgery programs then without an associated vascular surgery program, and 12 large private practice groups thought large enough to support a fellowship.
They tackled the issue at a critical juncture: since the inception of the integrated vascular surgery residency training paradigm in 2007 through 2015, the sum of new programs increased every year, Sheahan pointed out. Then the level essentially flat-lined for four years. “You can see that the number of new training programs stagnated around 0–2 a year. Since the initiative was started, we have 28 new programs. In the three years before the taskforce, we had seven programs total approved, then in the three years after we have 28 new programs,” he said.
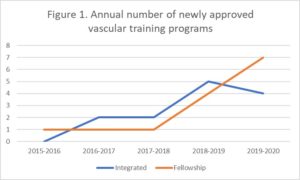
Four key planks of the initiative aided the taskforce efforts, Sheahan explained. First, they sought—and gained—clarification from the Residency Review Committee (RRC) of the Accreditation Council for Graduate Medical Education (ACGME) over faculty and program director requirements needed to start both an integrated program and a fellowship. They then set about providing stewardship to help guide those getting started through an often “byzantine and confusing” process, Sheahan said. They also increased outreach efforts through such mediums as a recurring Vascular Annual Meeting (VAM) session on how to start a vascular training program, the creation of an ad hoc APDVS committee to act as a home for continuing efforts, and one-on-one mentorship for new program leaders. Ultimately, the initiative worked, said Sheahan. Stressing more work remained to be done on the matter, “with a bit of a push, there are a lot of people out there who want to train vascular surgeons,” he added.
Private practice interest
Meanwhile, Sheahan’s data also showed that just two of the 12 private practices identified and contacted as potential sites for vascular fellowships expressed an interest in starting a program within the following three years, with the most common barriers cited being financial (50%), administrative (42%), and lack of interest (42%).
During post-presentation questions, this detail prompted Brigitte Smith, MD, program director of the vascular surgery fellowship at the University of Utah in Salt Lake City, to ponder whether private practices could partner with programs such as her own to increase opportunities.
“I have one spot a year for fellowship; could I offer two spots a year if I partnered with these private groups?” she asked “They don’t need to start their own program necessarily, but would they be willing to take trainees? That seems like a way to increase spots, if not programs.”
Sheahan explained that the absence of any kind of fellowship in the hospitals where the private practice surgeons operated appeared to be the main hold-up, alongside a gap in knowledge. “Part of it is still the RRC’s fault, in that how big some of these requirements are. So them clarifying in the last couple of years allowed a bloom in programs,” he said.
Responding to acknowledgment from the floor over recently successful Match seasons, Sheahan noted that the first two virtually administered interview processes during the pandemic for both integrated and fellowship programs saw 100% of positions filled—essentially a first. Earlier, Sheahan had conceded how when the question of vascular surgery training programs was looked at through the prism of “supply and demand,” he belonged to the demand side of the equation, arguing for a need to increase the number of students and residents in order to generate more programs. “We built all these programs but it seems like we are increasing demand as well,” he added during the question period.
Those operating outside of traditional training institutions potentially making a contribution to raising the level of trainee involvement in open aortic cases was the backdrop to O’Donnell’s data, which was garnered from the National Inpatient Sample between 2004–2015.

By looking at 140,000-plus cases, O’Donnell and colleagues at Beth Israel Deaconess Medical Center in Boston showed that some 38% of open AAA cases were performed at institutions classed as urban non-teaching hospitals, with 58% carried out in urban teaching locations and 4% at rural hospitals.
“Over time, open AAA volume in rural hospitals fell 89%, urban non-teaching volume dropped 87%, and urban teaching hospitals fell 58%,” he said. “At the end of the study period, rural hospitals accounted for 2.9% of open AAA volume, urban teaching centers 78%, and urban non-teaching hospitals 19%. However, in the last two years of our sample, non-teaching hospitals still accounted for almost 1,400 open repairs on average annually.”
O’Donnell continued: “Overall, mortality was 5%. There was no difference between teaching status in either group or in adjusted analyses. Despite concerning training experience with open AAA repair in recent years, a significant proportion of the open AAA repairs in the United States occur without any training participation. These data suggest that partnerships between vascular training programs and unaffiliated hospitals offer one potential solution to current deficiencies in open aortic training.”
Yet, bringing private practice vascular surgeons into the fold is not without challenges, members of the audience observed. Most of those practicing in non-teaching hospitals do so because they don’t want to perform cases with residents and fellows, said Linda Harris, MD, program director of the vascular fellowship and vascular residency programs at the University at Buffalo in Buffalo, New York. She also queried O’Donnell over how many open cases were realistically available at the 92 hospitals highlighted in the study, with the post-2015 period showing a sharp decline according to his research. “Based on the way of the trend, it’s probably about a thousand per year or so, maybe a little less than that,” O’Donnell said. “It’s a large opportunity; it’s certainly not every private hospital that will want to have residents come or fellows come. But any improvement is good, so we’ll take what we can get.”
In his capacity as an audience member, Sheahan chimed in to point out that aortobifemoral bypass surgery should be part of conversations about trainee involvement in open aortic surgery. “We have to get away from reporting open AAA as open aortic numbers, because they are not synonymous,” he said. “If you combine aortobifemoral and AAA, it’s not as dire as it looks. Yeah, open AAAs are going away, but we’re still doing a fair number of aortobifemorals, so consider that, too, when you publish.”
Robert Hacker, MD, a vascular surgeon at SSM Health in St. Louis, remarked that he would gladly cooperate with the teaching hospitals in the area to boost trainee exposure to open aortic surgery at his non-teaching urban medical center. “I’m really concerned that the people going to take care of me and you guys are not going to have the experience to do open,” he said. “Because as these aneurysms with endografts start failing, there’s no more metal to put in, and they’re going to have to be done open. I think you’re going to see a big mortality jump in a few years,” as surgeons at institutions like the Mayo Clinic start to retire, Hacker added. “I would strongly encourage the academic centers to reach out to the private and academic people like myself and develop relationships, because there’s a lot to be learned and lot of people who can teach.”
Gilbert R. Upchurch Jr., MD, a session moderator, brought the conversation to a close with a note on inroads being made. “We need to partner with people in practice. We’re doing that at the University of Florida,” he said. “We have a third fellow who’s going to be going down to work in Daytona. I know they’re doing this at SIU with conversations I had today. There is hope.”












