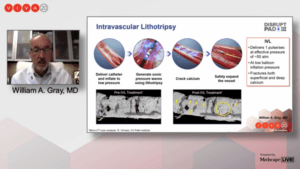
The DISRUPT PAD III randomized controlled trial (RCT) provides the largest level-one evidence for the treatment of heavily calcified femoropopliteal arteries, noted William Gray, MD, an interventional cardiologist at Main Line Health, Philadelphia, during the second and final late-breaking data session at this year’s Vascular Interventional Advances conference (VIVA 2020) held Nov. 6–8 virtually.
Gray reported that Shockwave’s intravascular lithotripsy (IVL) was superior to percutaneous transluminal angioplasty (PTA) in acute procedural success out to 30 days.
In addition, Gray informed the VIVA audience that IVL demonstrated atraumatic treatment, characterized by a reduction in percentage diameter stenosis prior to drug-coated balloon or stent placement, lower maximum inflation pressure, reduction in frequency and severity of dissections, and lower post-dilatation and stent implantation rate. He stressed that these RCT outcomes are similar to the PAD III registry in multiple vessel beds, highlighting the consistency of IVL treatment in complex anatomy.
Endovascular treatment of calcified peripheral artery lesions may be associated with suboptimal vessel expansion, increased complication risk, and reduced long-term patency. Single-arm studies have reported promising results with IVL in the presence of moderate and severe calcium, yet comparative evidence from randomized trials is lacking.
The purpose of this study is to compare acute outcomes in patients receiving vessel preparation with IVL or PTA prior to drug-coated balloon (DCB) treatment for peripheral arterial disease (PAD) in calcified femoropopliteal arteries. The DISRUPT PAD III RCT enrolled PAD patients with moderate and severe calcification in a femoropopliteal artery who underwent vessel preparation with IVL or PTA.
The primary effectiveness endpoint was procedural success, defined as core-lab adjudicated residual stenosis ≤30% without flow-limiting dissection prior to DCB or stenting. Secondary endpoints evaluated at 30 days included major adverse events (MAE) and clinically-driven target lesion revascularization (CD-TLR).
Gray detailed that in patients receiving IVL (n=153) or PTA (n=153), the primary effectiveness endpoint of procedural success was significantly greater in the IVL group (65.8% vs. 50.4%, p=0.007). Post-treatment balloon dilatation (measured prior to DCB) residual diameter stenosis (27.3±11.5% vs. 30.5±13.9%, p=0.04), freedom from any dissection (81.5% vs.67.7%, p=0.009), flow-limiting dissection (1.4% vs. 6.8%, p=0.03), and provisional stent placement (4.6% vs. 18.3%, p<0.001) were also significantly lower in the IVL group. Secondary outcomes, including rates of MAE and CD-TLR at 30 days, were comparable between groups.











