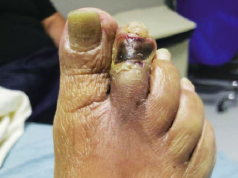
Four years ago, vascular experts from around the world were tasked with a quest to get all surgeons and providers to agree on the best ways to treat this common and debilitating illness: chronic limb-threatening ischemia (CLTI).
The goal came to fruition with the publication of the new global guidelines, produced by the European Society for Vascular Surgery (ESVS), the Society for Vascular Surgery (SVS) and the World Federation of Vascular Societies (WFVS) and published in the ESVS’ European Journal of Vascular and Endovascular Surgery as well as in the SVS’ Journal of Vascular Surgery.
CLTI is the end-stage of peripheral vascular disease, which carries with it the risk of amputation or even death from the effects of vascular disease.
The co-editors were Michael Conte from the SVS, Philippe Kohl from the ESVS and Andrew Bradbury from the WFVS. Nearly 60 additional authors worked on the project. Participants spanned six continents and represented all specialties that treat CLTI.
The collaboration between expert vascular specialists from around the world has created a unique practice guideline, reflecting the spectrum of the disease and approaches seen worldwide, said Conte. An extensive evidence review was undertaken, directed by a methodologist, to support the writing group’s work.
“This guideline provides a new foundation for describing and treating CLTI, an escalating public health problem around the world that involves a broad array of health professionals,” Conte said. “By improving the staging of CLTI, we believe that optimal care pathways can be defined and based on more accurate clinical and epidemiologic evidence going forward.”
Conte noted with pride that the multispecialty, international group of vascular experts emphasized the importance of a patient- and limbcentric approach to the care of CLTI.
“With the continuous evolution of vascular technology, we must remain focused on the primary goals of treatment, in contradistinction to a lesion-centric emphasis on technical success,” he said.
On the part of the ESVS, Florian Dick, of the University of Bern in Bern, Switzerland, spoke of a central message that approaches the patient in a holistic way—with a planned scheme. Speaking at the 2017 iteration of the ESVS meeting in Lyon, France, he went on: “Only then you can decide on how to treat the patients, as you have a basic matrix to predict risks and outcomes. Then you put in your differential treatments and you assess again. You have the chance to follow the patient in a very structured way, and make sure (i.e. measure) that what you are doing leads to improvement. If it does not, you change your treatment approach.”
Among the major changes that came with the new guidelines was to the name itself: The term “critical limb ischemia (CLI)” was “outdated” and failed to encompass the full spectrum of patients evaluated and treated for limb-threatening ischemia, the authors said.
Conte attributes the success of the diverse, international group to a process of consensus development. “A key aspect of our success was broad agreement on the importance of creating a new set point for CLTI around the world. CLTI is one of the most common conditions treated by vascular specialists, and often the most challenging. We also recognized that where evidence is limited the recommendations must be carefully considered to encompass the scope of practice,” he said.
Major recommendations cover the need for comprehensive assessments in patients with suspected CLTI; optimal medical therapy, including a variety of treatments for patients with CLTI; and prompt and effective revascularization for patients with advanced ischemia and limb threat. The document also outlines the importance of an individualized approach to improve patient care and reduce limb loss.
The guideline also endorses the SVS Threatened Limb Classification System based on grading Wound, Ischemia and foot Infection (WIfI) in the affected limb. And it introduces the Global Limb Anatomic Staging System (GLASS) to stratify the patterns of arterial occlusive disease in the affected limb. GLASS integrates the complexity of disease along a selected target artery path from groin to foot. GLASS stages (1–3) are designed to correlate with immediate technical success and 12-month limbbased patency following peripheral vascular intervention.
The GLASS classification, explained Dick, “really relates to the arterial path down the limb. After the step back to see the holistic scheme which integrates the person and the problem (wound, perfusion and infection), you need to go into more detail for the anatomic scheme of the arterial path. With GLASS, we have a matrix that assesses the two levels (fem-pop and tibial) regarding arterial vascularization options with the aim of restoring one path to the foot. Essentially, GLASS looks at the distribution and the severity of the different lesions along the whole limb, and grades them against the chances of success with endovascular treatment.”
Conte highlighted the guideline’s “structured approach to decisionmaking regarding revascularization based on patient risk, limb severity and anatomic complexity (PLAN), in that order of priority,” adding that it “seeks to provide a new foundation for practice but also for data collection to support evidence-based revascularization in CLTI.”
Beyond improving patient care, identifying key research priorities is an important secondary goal for the guideline. Thus, each section includes such priorities, where efforts and resources should be focused to improve patient care and advance the science.