Speaking at the Virtual Aortic Surgery How to Do It Highlights conference (Dec. 17–18), Stéphan Haulon, MD, a vascular surgeon at Hôpital Marie Lannelongue, Paris, France, discussed total endovascular treatment of the aortic arch in chronic dissections.
Detailing global experience using three-vessel inner branch stent grafts for this procedure, Haulon highlighted good technical success and low morbidity and mortality rates. However, he also stressed that the high number of secondary procedures required remains the “Achilles’ heel” of the technique, and that larger experiences and longer follow-up are mandated.
Before delving into the use of arch branch devices in chronic dissections, Haulon made it clear that it was not his intention to take part in the debate between open versus endovascular surgery in this presentation. He detailed his reason: “Patients that have a large ascending aorta cannot be treated with [arch branch devices].” Instead, his focus was on those patients for whom endovascular treatment was feasible.
Moving on to the “evolution” of arch branch device design, Haulon noted that this began a long time ago with fenestrated endografts, before surgeons moved towards using the single branch and subsequently the inner branched design. Honing in on this latest iteration, Haulon informed viewers: “The nice thing about [the inner branched] design is that you have a tapered portion in the middle where the branches are positioned, so you always have flow to the supra-aortic trunk.”
Focus on patients with chronic dissection sees drop in stroke rate
Haulon communicated that he and colleagues started using arch branch devices over 10 years ago to treat atherosclerotic aneurysms, noting that their initial experience was not good, with a 15% stroke rate. However, he added that better results have followed a switch from treating atherosclerotic aneurysms to treating chronic dissections—patients that had a prior type A repair who required a follow-up procedure due to false lumen evolvement in the arch and in the descending thoracic aorta, he explained.
“The main reason for getting a good outcome,” Haulon stated, “is that we now had a perfect landing zone, which in many of those patients is a long, proximal tube,” and no (or less) atherosclerotic plaque on the aortic wall. However, he added that some of those patients will have either a short or a kinked tube, meaning they cannot be treated.
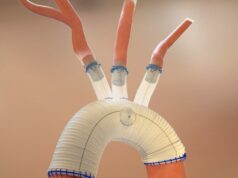
In the specific anatomy of a chronic dissection of the arch, Haulon detailed that most patients are “perfect” candidates for the new arch branch device design—the three-branch endograft with a retrograde branch perfusing the left subclavian artery.
Haulon then considered the outcomes of patients with a chronic dissection who have been treated with inner branched arch endografts following ascending open repair.
In a retrospective international multicenter study published in the Annals of Surgery in 2019, Dorian Verscheure, MD, also of Hôpital Marie Lannelongue, Haulon and colleagues looked at 70 patients across 13 vascular units in nine countries who obtained “unmatched” results—a combined in-hospital mortality and stoke rate of 4% and a “very high” technical success rate of 97%. “It was really interesting to see that, compared to the initial 15% stroke rate, we went down to 4% by focusing on those patients with chronic dissection,” he remarked.
Number of secondary procedures represents “Achilles’ heel”
Despite these improved results, Haulon stressed that there is an “Achilles’ heel” to this procedure—the number of secondary interventions required. He noted that most of these are due to persistent flow in the false lumen, requiring either coil embolization in the false lumen or an extra-anatomic bypass of the supra-aortic trunk. Here, Haulon referenced the work of Tilo Kölbel, MD, a vascular surgeon at University Hospital Eppendorf, Hamburg, Germany, who advises getting a complete exclusion by implanting a candy-plug in the distal false lumen.
Finally, Haulon referenced a presentation given at this year’s SVS ONLINE meeting (June 20–July 2) given by Emanuel R. Tenorio, MD, of the Mayo Clinic, Rochester, Minnesota, on a multicenter global early feasibility study that gathered all the three-branched data, including mainly patients with a dissection. He noted the technical success rate of 100%, a combined mortality and stroke rate of 8%, and a 5% 30-day mortality, but again, a high secondary procedure rate—around 60%.
Concluding, Haulon stressed that this multicenter global experience demonstrates the technical feasibility and safety of total endovascular aortic arch repair for aneurysms and chronic dissections using three-vessel inner branch stent grafts. Mortality and stroke rates compare favorably to reported outcomes of total open surgical arch replacement, he summarized, particularly among higher risk patients who had prior median sternotomies and ascending aortic repairs.
However, Haulon reiterated that a limitation remains the high rate of secondary interventions, and—while these are planned in most cases—stressed that “this is something that needs to be shared with the patient”.