
The prospect of remote stroke intervention may be the most exciting clinical application among the suite of benefits emerging from the ongoing transformation in surgical practice and education delivery, Alan Lumsden MD, the medical director of Houston Methodist DeBakey Heart & Vascular Center in Houston, will tell viewers during this year’s iteration of the Roy Greenberg Distinguished Lecture.
Lumsden is giving the address—entitled “TeleWhat? Beyond the office: How remote support systems will transform education, case support and care delivery”—on the second day of SVS ONLINE, Tuesday, June 23, at 6 p.m., as the digital alternative to the canceled Vascular Annual Meeting (VAM) moves onto Scientific Session 2 and its first Invited Session, “American Venous Forum Debates 2020: Are DVT & PE interventions unnecessary?”
Having the ability to perform a procedure from afar is the “holy grail” among these remote support systems, the professor of cardiovascular surgery is set to say during the lecture, against the backdrop of a COVID-19 pandemic that not only caused VAM 2020’s cancelation but also a surge of interest in telemedicine.
Lumsden will connect the dots that unite a modern era in which boundaries are being pushed in the delivery of education, case support and care.
“The COVID-19 epidemic dramatically increased interest in telemedicine,” he told Vascular Connections in the days leading up to the start of SVS ONLINE. “However, for most, this simply means tele-consultation in an office-based environment. In this presentation we’re going to study some of the more advanced applications that are specific to surgical practice. Specifically, how remote audiovisual platforms can be employed for case support, remote monitoring, remote education and potentially perform remote interventions.”
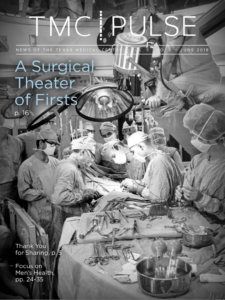
Lumsden points to an old picture published on the cover of TMC Pulse in July 2018—depicting the operating room of the late vascular surgeon Michael DeBakey, MD—as a yardstick of progress.
“In this black and white picture from Dr. DeBakey’s operating room, you see old-style surgical education with people crowding around,” he said. “If you look up above the field, there is a huge television camera with someone lying on the boom to record the case. If you look even higher, there are viewing domes where folks could attempt to see down into the wound. Clearly, technology has moved on, and contemporary audiovisual communications systems potentially allow us to transform case support. This is something I have long had a keen interest in.”
Lumsden will first train his focus on advances in medical education. “Education has clearly been transformed, in some ways for the better and many others for the worse by the COVID-19 crisis,” he continued. “Everyone has discovered Zoom. There is now a plethora of online offerings associated with the rapid development of Zoom fatigue. This makes it hard to differentiate oneself from the crowd. It is particularly a challenge in developing a hands-on curriculum. We recently designed an online hands-on curriculum for the upcoming vascular intern class.”
The hands-on tradition was something Lumsden and his colleagues wanted to continue. “For the first time ever, we believe, a remote course focusing on basic suture skills was conducted, in which sewing kits were distributed to all 57 participants,” he explained. “Demonstration by and supervision from remote proctors was achieved in small classes of four to five students. Optimization of a CT [computerized tomography] image and working in the MPR [multiplanar reformation] environment was performed by distributing standardized CT scans and software to all the students. These are but two examples of how surgical training may have to adopt to our new reality.”
Support for acute cases, meanwhile, was brisk.
“When the epidemic hit, we could immediately deploy many of the remote systems in support of acute cases,” said Lumsden. “We had requested that the device reps familiarize themselves with remote support, practice with the interface and gain an understanding of the benefits and limitations of this technology. Although many of these systems are fairly easy-to-use, it is important that users familiarize themselves with the interface through practice before covering emergent cases. Remote support was used in at least three emergent cases during the COVID-19 crisis. This led to a degree of acceptance, which has now extended into elective cases.”
But lessons have been learned, too. “With use, it has become apparent that optimization requires attention to bandwidth, camera positioning, the audio communication system and the format of verbal communications,” Lumsden added. “In addition, the number of video feeds which are necessary is case-specific.”
It’s remote support’s “holy grail,” though, that gets the Houston Methodist’s Walter W. Fondren III Distinguished Endowed Chair particularly excited: the carrying out of actual procedures.
“This has been successfully demonstrated, with the first case being remote coronary intervention in India, and the second being a neurointervention in Toronto,” Lumsden noted. “Many of the prerequisites for good audiovisual communication are also intrinsic to remote catheter control. We will demonstrate early data on performing remote endovascular interventions in a simulated environment. Remote stroke intervention may be the most exciting clinical application—a high public health need where the efficacy of early intervention can have massive health and economic implications. In the end, it is all about speed of data transmission, reliable audiovisual communication and case choreography between observer/operator and the patient.”












