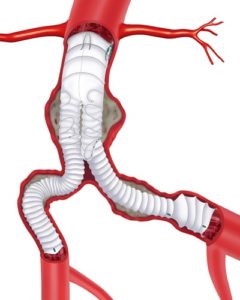
The third-generation Anaconda endograft from Terumo Aortic provides “high technical success” as well as “satisfactory” five-year aneurysm exclusion and clinical success rates, a French multicenter prospective observational study has found.
The investigators note that longer-term results with new generation endografts are “essential” due to a significant decrease in aneurysm-related survival observed in long-term follow-up after infrarenal endovascular aneurysm repair (EVAR) compared with open repair.
A total of 176 consecutive unruptured infrarenal abdominal aortic aneurysms (AAAs) between June 2012 and October 2013 were included in the study (160 male patients, mean age 75.3±8.4 years). Survival, freedom from type Ia endoleak, limb events and reinterventions were estimated using the Kaplan–Meier method, and anatomical and clinical characteristics were compared according to the occurrence of migration, conversion, adverse limb events, endoleak, and sac enlargement.
The findings, which were published by Dominique Midy, MD, of Groupe Hospitalier Pellegrin in Bordeaux, France, et al in the European Journal of Vascular and Endovascular Surgery (EJVES), showed primary technical success was 98.3% and clinical success was 94.9%. A hostile neck was identified in 33.9% of patients and 10.7% were treated outside the instructions for use (IFU). An early postoperative (≤30 days) mortality rate of 1.7% was observed. At one and five years, respectively, the overall survival rate was 94.9% and 65.9% (aneurysm related in four patients [2.3%]) and the clinical success rate was 90.9% and 70.6%.
Secondary interventions were performed in 35 of 176 patients (19.9%). The overall limb occlusion rate was 7.9% and the aneurysm sac diameter decreased significantly (preoperative diameter 53.9±8.6 mm vs. 42.3±14.7mm at five years; p<0.001). Patients treated outside the IFU had significantly higher rates of migration, surgical conversion, and aneurysm sac expansion (p=0.03).
The investigators also stressed that implantation outside the IFU “should be avoided” as it leads to “significantly worse outcomes,” adding that “caution over the risk of limb occlusion and distal embolization should be observed.”
SOURCE: doi.org/10.1016/j.ejvs.2020.02.005












